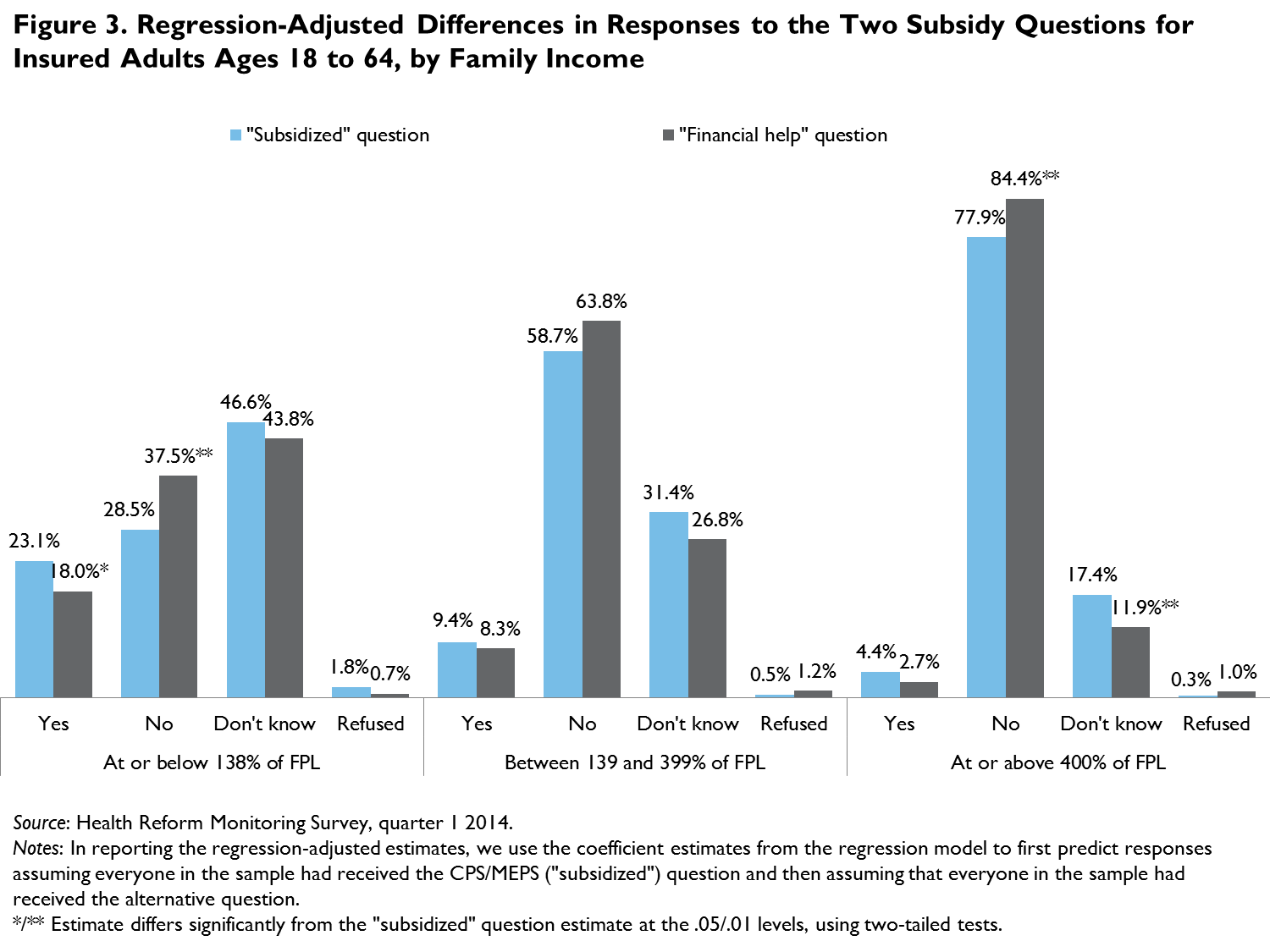QuickTake: [How] Should We Ask about Premium Subsidies in Household Surveys?
Sharon K. Long, Victoria Lynch, Joanne Pascale, Kathleen Thiede Call, Lisa Clemans-Cope, and Michael KarpmanDecember 2, 2015
The Affordable Care Act (ACA) is significantly changing the share of nonelderly adults who are obtaining subsidized health insurance coverage, both through the Medicaid expansion and through qualified health plans in the new health insurance Marketplace (Centers for Medicare and Medicaid Services 2015; Office of the Assistant Secretary for Planning and Evaluation 2015). Accurately measuring enrollment in these new subsidized coverage options is critical for assessing these new programs. Although administrative data can provide data on enrollment, survey data can provide an in-depth understanding of the characteristics and circumstances of enrollees. But asking about participation in subsidized coverage through household surveys is challenging because of the complexity of our system of public and private coverage, in turn making it difficult for researchers to design effective survey questions and difficult for survey respondents to answer those questions. Those issues are likely amplified by the increasing complexity of both the health insurance system and the complexity of the process for determining subsidies, as well as confusing subsidy terminology. In the March 2014 Health Reform Monitoring Survey (HRMS), we tested two alternative survey questions in a randomized experiment to explore how to ask about premium subsidies in a household survey. One question was based on the language used in the Current Population Survey (CPS)/Medical Expenditure Panel Survey (MEPS),1 and an alternative question was based on wording proposed by an expert panel:
In the experiment, one-half of nonelderly adults ages 18 to 64 who reported that they had health insurance coverage at the time of the survey were randomly assigned to be asked the CPS/MEPS question and one-half were randomly assigned to be asked the alternative question. Table 1 shows that the characteristics of the two random subsamples were quite similar and differed only in the share of the adults who reported very good or excellent health. In reporting the results, we focus on regression-adjusted differences that control for the measures included in the table. As would be expected given the similarity of the split samples, the simple differences and regression-adjusted differences are quite similar.
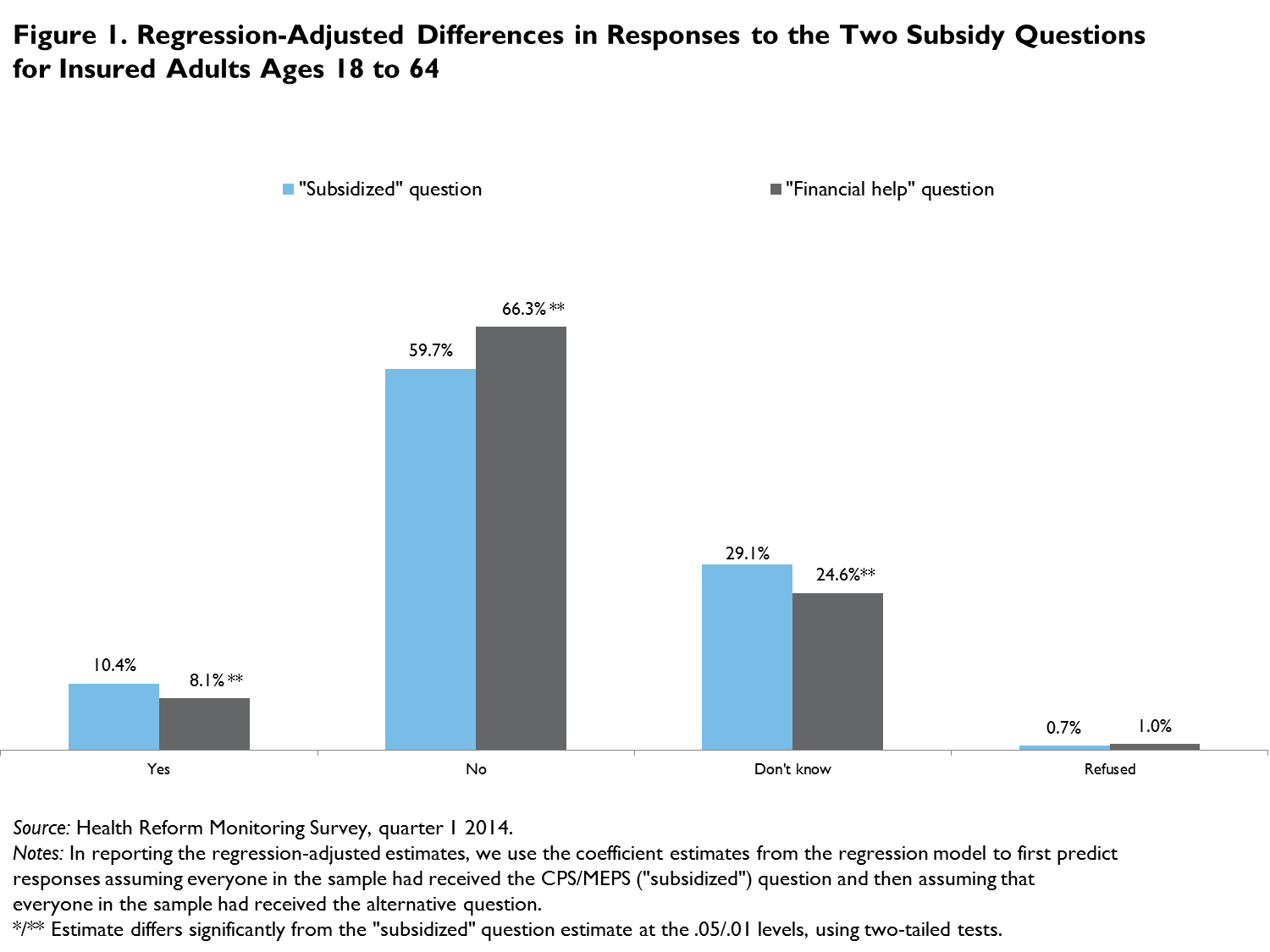
As shown in figure 1, we find that, after adjusting for differences in the characteristics of the random samples, somewhat more of the insured adults reported they had a subsidy (10.4 versus 8.1 percent) and somewhat fewer reported that they did not have a subsidy (59.7 versus 66.3 percent) based on the CPS/MEPS “subsidized” question relative to the alternative “financial help” question. Of concern, however, 29.1 percent of the insured adults reported that they did not know the answer to the CPS/MEPS question and 24.6 percent did not know the answer to the alternative question.
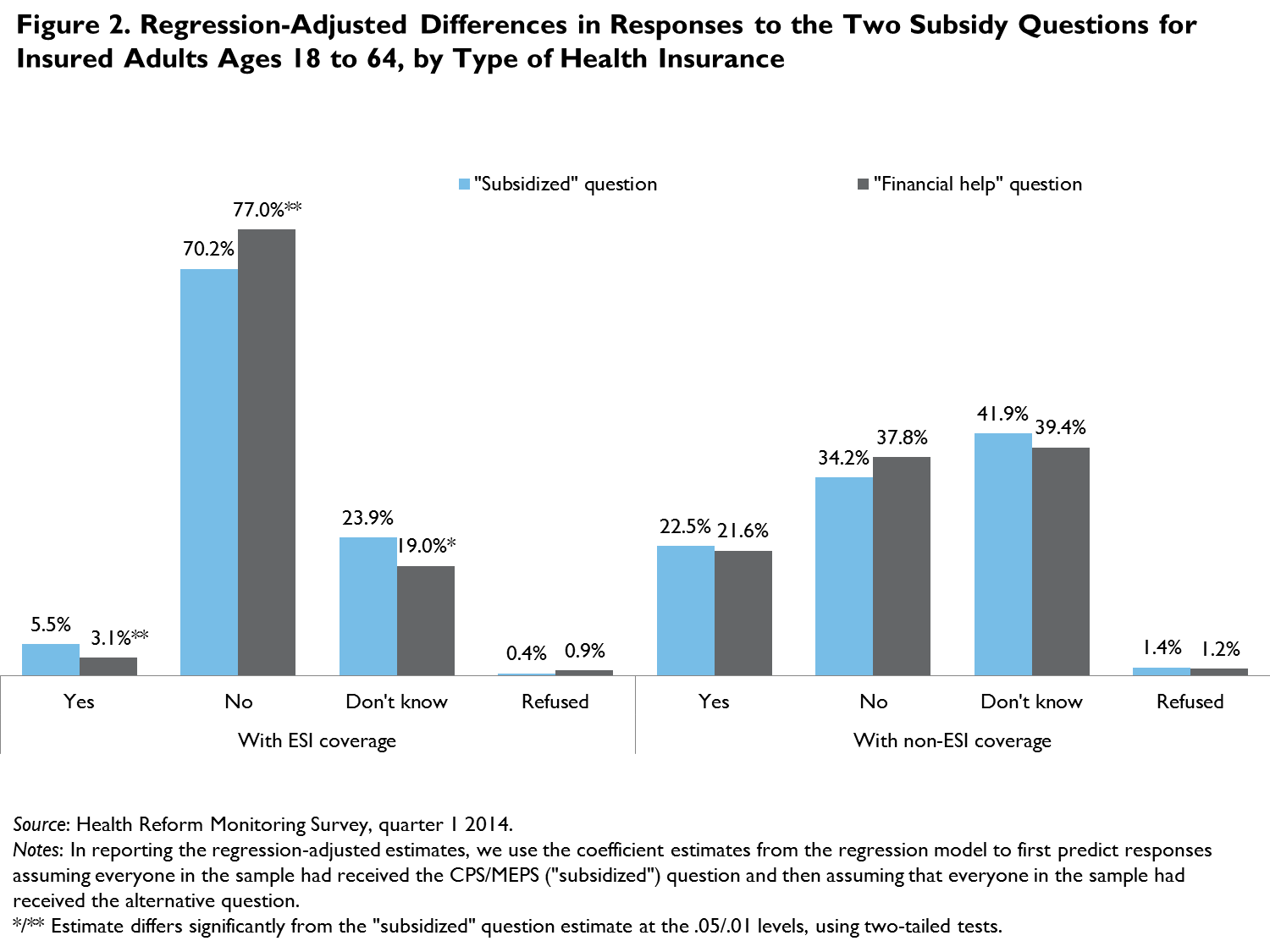
Similarly, when we limit the sample to adults in the income groups targeted by the Medicaid expansion and the Marketplace, responses are more consistent across the survey questions, particularly for those targeted by the Marketplace subsidies, where there are no statistically signficant differences in responses to the two questions (figure 3). Again, however, the share of adults reporting that that they did not know the answer to the subsidy questions is high: more than a quarter responded as such to both the “subsidized” question and the “financial help” question.2
Conclusions
The findings from a random experiment in the HRMS that tested two approaches to asking about subsidized health insurance coverage suggest that as of March 2014, question wording could matter, although much less so among the population group targeted by the ACA’s Marketplace subsidies. Regardless of question wording, however, many respondents were confused as to whether they have a premium subsidy, with large shares reporting “don’t know” even among the income group targeted by the Marketplace subsidies. Although this study does not identify whether respondent confusion stemmed from confusion about the characteristics of their health insurance coverage, confusion about program terminology, or confusion with question wording, the findings suggest a need for caution in interpreting results from current questions about receipt of subsidies for health insurance premiums in household surveys. This study also suggests a need for additonal research both into methods of targeting subsidy questions to the respondents for whom they are potentially relevant and into comparisons of responses to survey questions with adminstrative data on actual subsidy receipt.
References
Centers for Medicare and Medicaid Services. 2015. Medicaid & CHIP: July 2015 Monthly Applications, Eligibility Determinations and Enrollment Report. Baltimore: Centers for Medicare and Medicaid Services.
About the Series
For more information on the HRMS and for other QuickTakes in this series, visit www.urban.org/hrms.
Notes 1 Because the HRMS did not include questions on premiums that precede the CPS/MEPS questions, we added the phrase “for your health insurance plan” to the version of the question in the HRMS. 2 Small sample sizes prevent us from splitting the sample by both coverage type and family income to more closely target the target population for subsidies under the Marketplace.
|
||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||||